
Breathing Mechanics and Physiology: Why Better Breathing Means Better Health
We breathe over 20,000 times a day, yet most of us don’t think twice about it. But if you struggle with chronic pain, fatigue, stress,

Given that physical activity is the ultimate remedy to staving off many lifestyle diseases including OA, this is a big issue.
If Osteoporosis is the disease of bone being taken away, Osteoarthritis can be thought of as the disease of bone being laid down. That is, as your cartilage thins or degrades due to various factors it isn’t as effective in its shock absorbing role, so bone takes over.
Bone lays down according to lines of stress, if there is more stress, more bone is laid down, if there is less stress and load, bone is resorbed and taken away.
Physiology at its most basic here.
Of course, there are many factors that influence bone production and resorption but this is one of the most fundamental laws governing what is happening at this level.
The other important factor in our physiology is that there are many mechanical components that make up our articular or joint cartilage. Our collagen fibres in our cartilage can degrade with too much load or after an injury but we can build and maintain the resilience of what is left.
We can optimise the function of our cartilage.

Understanding this means that what has been commonly thought of about Osteoarthritis, that it is all downhill from here, is not necessarily the case at all.
Osteoarthritis can no longer be thought of as simply wear and tear – that you have worn the joint out. Yes, in severe cases this can happen and joint replacement surgery is necessary and thankfully available to us but this severity generally takes decades to develop if it is going to develop at all.
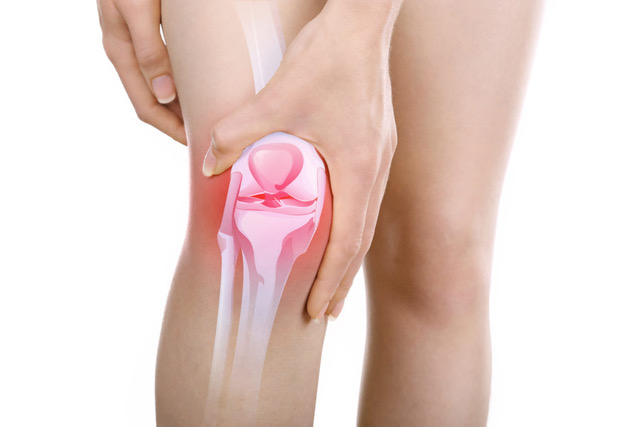
Unlike rheumatoid or other systemic inflammatory conditions of the body that can affect our joints, OA tends to have a mechanical reason for being, however, genetics can play a part in whether you are likely to develop Osteoarthritis and inflammatory processes are accelerated in people who are overweight through mechanisms that aren’t completely understood.
There are many reasons but we can simplify it down to optimal loading and cartilage durability.
We need it just right!
You can think of cartilage as a sponge.

When you compress it with a load, say with a squat, the synovial fluid moves out of the cartilage. When you take the load off when you stand back up again, special proteins within the cellular matrix called proteoglycans resorb the fluid back into the cartilage.
Too much load and you just squeeze all the fluid out without giving it a chance to resorb, not enough load and you don’t get the adequate movement of fluid in and out.
We are always turning over cells and renewing in our bodies and our cartilage is no different.
Without a blood supply this process is slower in cartilage but it still happens. We are constantly in a cycle of regeneration and degradation. The key is to make sure you are in balance with this so regeneration cancels out degradation. Similar processes occur with bone and osteoporosis.

Everyone is different.
For some, training for and running a marathon is a perfect load for their joints (though they are in the minority ).
For others walking 30 mins every day is just the right load but if they do a big bush walk on the weekend without getting used to this step up in load, this might tip them over.
Others whose joints are displaying signs and symptoms of OA may have to modify their load and find a walk every second day is best for them supplemented with a bike ride another day or a group fitness class another.

In over 20 years of teaching classes for people with all sorts of issues, I have been bowled over as to how well knees and hips respond to exercise that in years gone by would have been on operating lists for replacement surgery well before. They get better, not worse. And when and if surgery is required they are well placed for the recovery stage as they have the strength and coordination ready to go.
Optimal alignment is also key when it comes to optimal loading. This is where your physiotherapist and/or supervised exercise classes can help to ensure you are aware of how to optimally load your body with optimal alignment and movement patterns.

In a pyramid diagram representation of what is recommended for people with arthritis, exercise, diet and education are the first line defence. Second comes medications including Panadol and Anti-inflammatories, hands on modalities including massage, joint mobilisation and acupuncture as well as supports like orthotics and aids. The third tier is left for surgery.
Just like most lifestyle diseases, what we put in our mouths makes a huge difference to how our bodies are. Certain foods are inflammatory. Research has shown that the Mediterranean diet has strong anti-inflammatory properties as well it is recommended by CSIRO for long term weight loss. High in vegetables and omega 3 containing foods like fish and nuts, it assists your body to in putting out the fires of inflammation and halt it coming on in the first place.
Chatting to a nutritionist about your diet can be life changing. Simple little changes you can make on a daily basis can make a huge difference to how you feel now and in the future.
Over the last few decades, research has been growing exponentially regarding the neuroscience behind pain particularly how this relates to what we are seeing on scans.
With OA, changes on X-Ray and scan often take decades to develop, yet the pain and stiffness associated with joint changes occurs much earlier.
Waiting until there is a diagnosis through X-Rays doesn’t make sense when we can be doing so much to help our joint health now.
Also, many people are coming to this understanding more and more that what we see on scans doesn’t necessarily correlate well with pain. That is, some people have little pain but their scans can look downright terrible like this one. Others experience a lot of pain with minimal to no changes on their scans.
It can tell us when the load is too high, or we are in the wrong position or we need to change what we are doing. It doesn’t necessarily mean we need to stop what we are doing.
A really good guide is that it is safe to exercise at 2/10 pain (where 10/10 is excruciating pain and 0/10 is no pain at all) up to 5/10 so long as any pain subsides within 24 hours. Again, utilising the experience of your physiotherapist can help you to discern what level of exercise is right for you and how to progress and get stronger safely.
So, when it comes to the most common questions regarding Osteoarthritis,
NB: a lot of the information presented above has derived from the amazing work of a fabulous group of researchers who developed the GLA:D program (Good Life with Arthritis: Denmark). I am a registered GLA:D practitioner and have had the good fortune to be involved with the program for the last 3 years. The program initiated in Denmark, was translated in Canada and brought out to Australia by Monash University. For access to further great information on Osteoarthritis visit www.gladaustralia.com.au and/or join us for our OA workshop these school holidays.


We breathe over 20,000 times a day, yet most of us don’t think twice about it. But if you struggle with chronic pain, fatigue, stress,

From Melinda… For people who come to my classes and clients who have been seeing me for a while, may have heard some of the

Meet Susan Susan recently suffered a fall attempting to lift a 2.5kg bag of soil overhead in her garden shed when she felt her leg
Sign Up Below To Get Your Free RedoHealth Guide Now

By registering, you agree to receive SMS and email communications from RedoHealth. No spam guaranteed. Unsubscribe at anytime.